Similar expressions
CT contrast brain/ CECT brain/ CT brain contrast
Introduction
Brain contrast scan is performed mainly to assess benign and malignant neoplastic conditions associated with the brain. Iodinated contrast media is used intra venously (IV) to enhance lesions.
Patient preparation
- Remove hair clips, ear rings or any removable metal in the exposing area.
- Explain the procedure clearly.
- Ask the patient to be steady during the acquisition.
- Check contraindications for contrast media administration and radiation exposure.
- Place an intra-venous cannula – pink color or 20 Gauge cannula.
Patient positioning
- Position the patient in supine and head first.
- Position the head in the head rest.
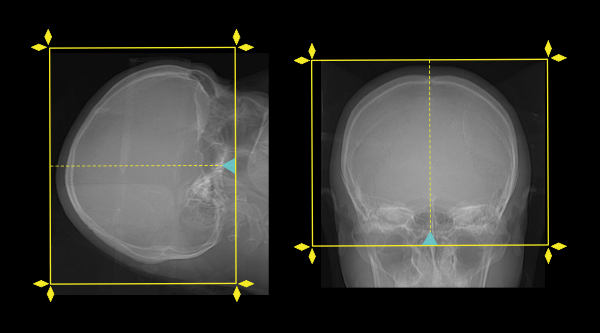
- Tilt the patient’s head so that the line joining supra-orbital point and external auditory meatus(EAM) perpendicular to the floor, and ask to close the eyes.
Explanation: This method reduces the eye lens dose (if you need more references and images related to this, please refer to our brain non-contrast article).
- Immobilize the head using a strap.
- Center the scanning area in the scanner iso-center.
Explanation: this reduces overall radiation exposure and increases image quality [1].
Scan planning
- Plan the scout start point (laser indicator) at the upper lip of the patient.
- Plan the scan slab from the skull vertex to skull base for both pre- and post-contrast scans.
- Perform a pre-contrast scan.
- Inject 50ml (for a patient with 50 to 60kg of body weight) of iodinated contrast media.
Explanation: hand injection is the common method. Pressure injector, however, can be used with a lower injection rate (1ml/s).
- Perform a post-contrast scan nearly after 5 minutes from the contrast injection.
Post-processing
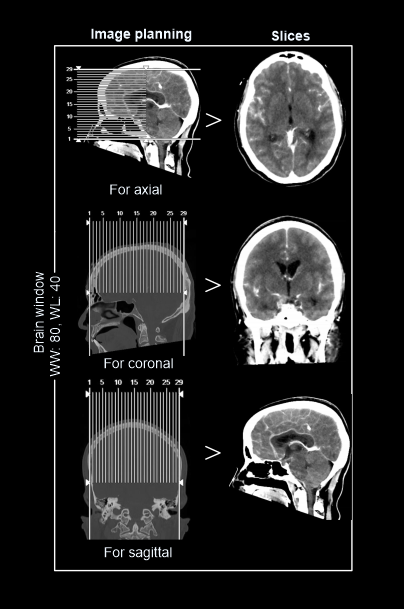
- 5 mm axial images in brain window (WW80, WL40) of both pre and post contrast images.
- 1-2mm axial, coronal or sagittal images of the skull in bone window (WW3500, WL350) to show fractures, dislocations or bony abnormalities.
- 3d images to show abnormalities.
Please view bone window images in brain non-contrast article.
Reference
- Romanyukha, A., Nzitunga, P. S., & Dolcet, A. (2022, April 28). CT patient positioning plays key role in radiation dose reduction. www.auntminnie.com.
- Blackham, MD, Chair, K., Jordan, MD, FACR, J., & Corey, MD, FACR, A. (Eds.). (2020). ACR–ASNR–SPRPractice parameter for the performance of computed tomography (CT) of the head.
- Tamangani J. Neuroimaging. Aust Fam Physician. 2016 Nov;45(11):788-792. PMID: 27806446.
- Abbasi, B., Ganjali, R., Akhavan, R., Tavassoli, A., & Khojasteh, F. (2023). The accuracy of non-contrast brain CT scan in predicting the presence of a vascular etiology in patients with primary intracranial hemorrhage. Scientific reports, 13(1), 9447.
- Dieckmeyer, M., Sollmann, N., Kupfer, K., Löffler, M. T., Paprottka, K. J., Kirschke, J. S., & Baum, T. (2023). Computed Tomography of the Head: A Systematic Review on Acquisition and Reconstruction Techniques to Reduce Radiation Dose. Clinical neuroradiology, 33(3), 591–610.